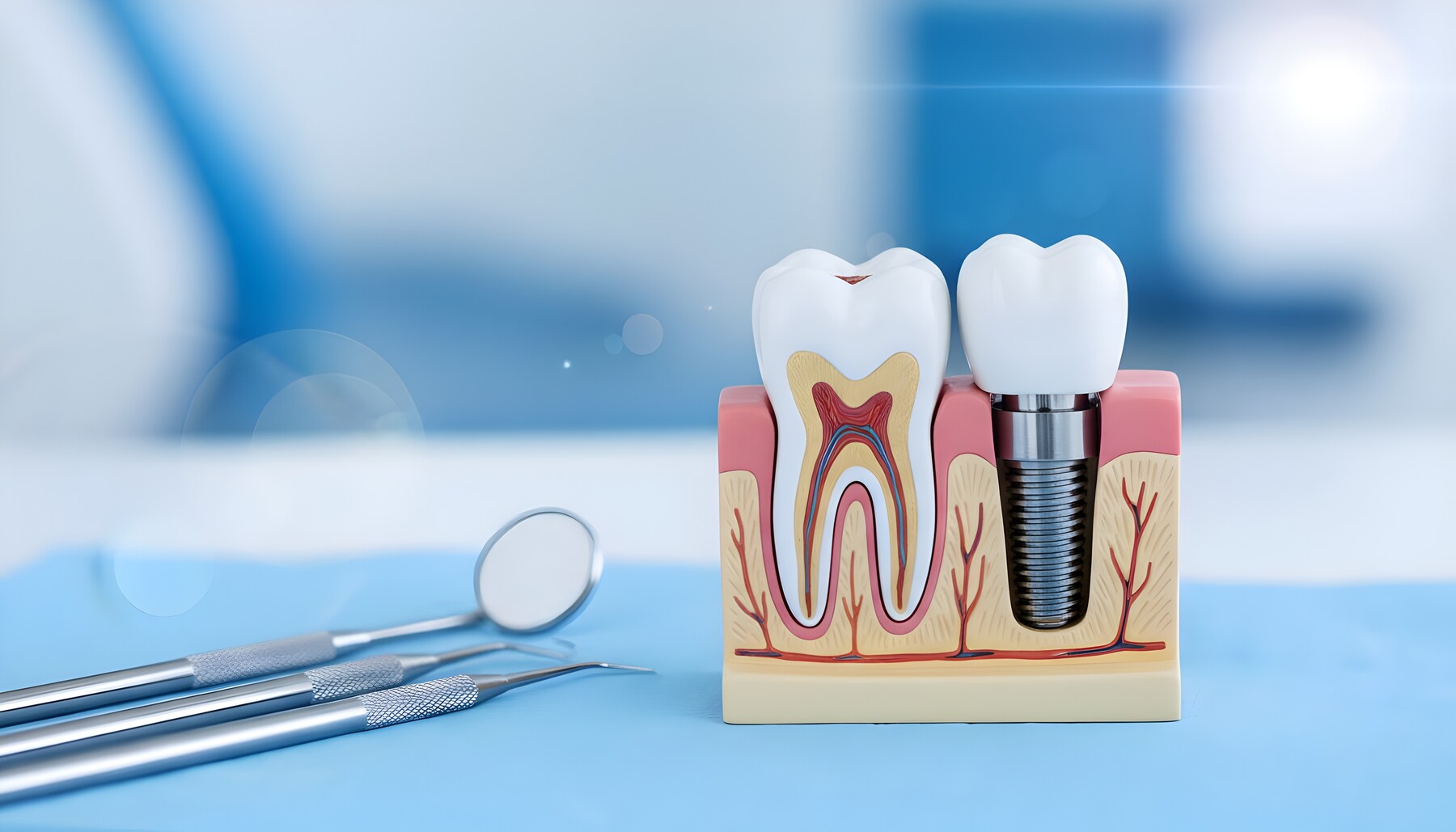
If you’ve been wondering whether you’re a candidate for dental implants, here’s the reassuring answer: many adults are. Implant candidacy usually isn’t about having a “perfect” mouth. It’s more about whether your gums, bone, and overall health can support healing well. In other words, this isn’t a pass-or-fail test. It’s a planning conversation.
A simple checklist: signs you may be a good candidate
You may be a strong candidate for dental implants if most of these sound like you:
- You’re missing one or more teeth and want a stable, long-term replacement.
- Your gums are healthy, or you’re willing to treat gum disease first. Healthy gum tissue matters because implants rely on the surrounding soft tissue and bone for support.
- Your gums are healthy, or you’re willing to treat gum disease first. Healthy gum tissue matters because implants rely on the surrounding soft tissue and bone for support.
- Your general health is reasonably stable. Good health supports healing, and age by itself usually matters less than your overall health history.
- You’re willing to keep up with home care and regular checkups. Implants still need brushing, cleaning around them, and professional monitoring.
The “let’s plan around this” list
Some factors aren’t hard no’s. They’re more like yellow lights that tell us to slow down, look a little closer, and build the right plan first. That might mean treating gum disease, improving home care, reviewing medications, or doing bone grafting before implant placement.
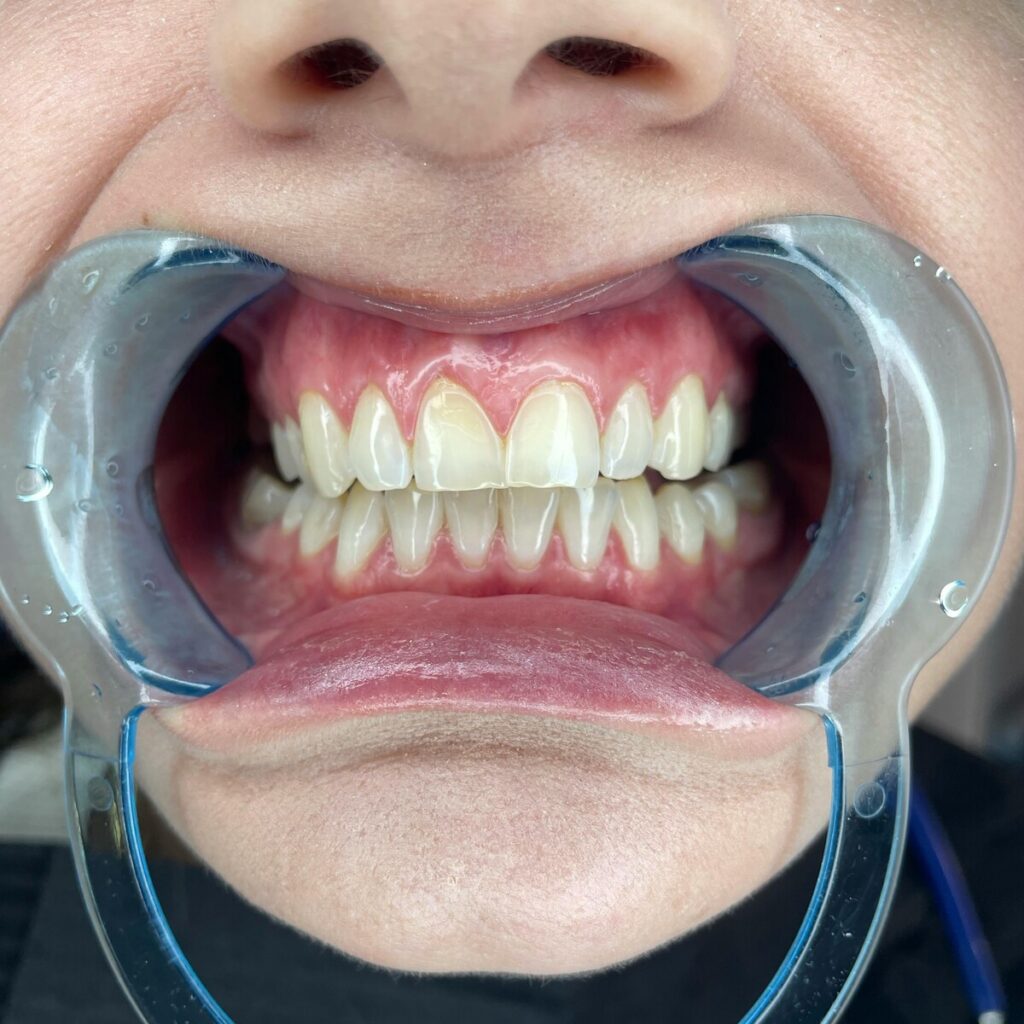
Gum health comes first
One of the biggest green lights is healthy gum tissue. If your gums are inflamed, bleeding, or affected by active periodontal disease, your dentist will usually want to get that under control before placing an implant. That’s not a punishment, and it doesn’t mean the conversation is over. It’s simply the smartest way to protect your long-term result.
A history of periodontitis also deserves an honest conversation. Research shows that patients with a history of periodontitis can have higher risks of implant failure, peri-implantitis, and greater bone loss around implants. That doesn’t mean implants are off the table. It just means you may need a more customized maintenance plan.
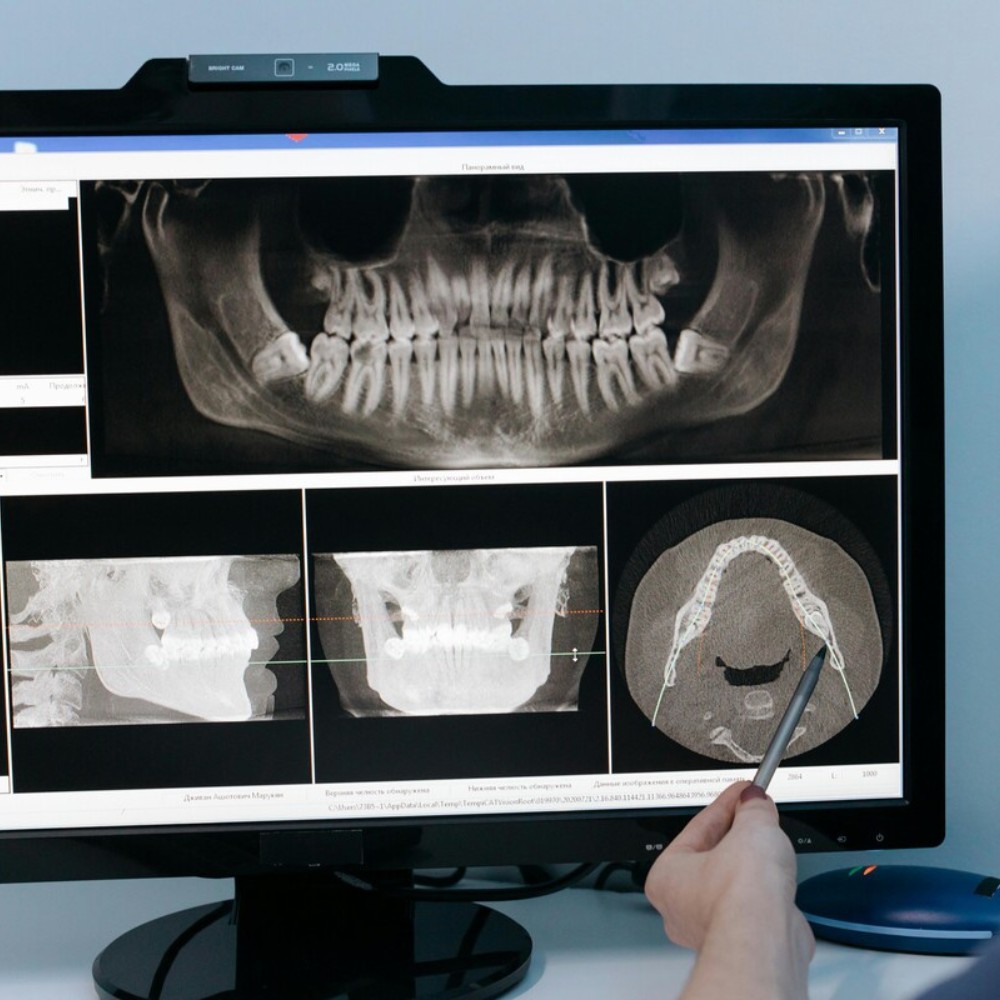
Bone matters, but low bone doesn’t always end the conversation
Implants need enough jawbone for support. If a tooth has been missing for a while, that area of bone can shrink over time. The good news is that low bone volume doesn’t automatically rule you out. Many patients can still move forward with bone grafting or other preparatory treatment to build a stronger foundation first.

Health history matters more than people think
Your consultation should include a real review of your medical history, medications, and any conditions that could affect healing. This is especially important for issues tied to bone healing or infection risk. The goal isn’t to look for reasons to say no. The goal is to make treatment safer and more predictable.
Diabetes is a good example. The research is more nuanced than many people expect: controlled diabetes isn’t automatically a deal-breaker, but poorly controlled diabetes is associated with more peri-implant problems and higher long-term implant loss. So if you have diabetes, the question usually isn’t, “Can I never get implants?” It’s more often, “How well controlled is it, and how do we plan around it?”

Habits can affect healing too
Smoking and nicotine use are worth discussing without shame or lectures. This isn’t about being judged. It’s about healing. Major patient and clinical sources note that smoking can interfere with healing, and systematic-review evidence shows a significantly higher implant failure risk in smokers than in non-smokers. If you smoke, your dentist may recommend quitting or cutting back around treatment to give the implant a better chance to succeed.
Teeth grinding is another habit worth mentioning. It doesn’t automatically make you a poor candidate, but it may mean your dentist recommends extra protection, such as a nightguard, so the implant and restoration aren’t taking more force than they should.
What your implant consultation usually checks
A dental implant consultation often includes a full exam, imaging or 3D scans, a review of your bite and gum health, and a conversation about your medical history and goals. This is how your dentist figures out whether you’re ready now or whether a few preparatory steps would improve your outcome. Think of it less like being “judged” and more like creating a blueprint.
The Bottom Line
If you’re wondering whether you’re a candidate for dental implants, don’t assume the answer is no just because you’ve had gum disease, bone loss, diabetes, or a few dental complications in the past. Many people are ready for implants right away. Others become excellent candidates after a little prep work. Healthy gums, enough support, good home care, and thoughtful planning are usually what matter most.
To learn more, explore our Dental Implants and Restorative Dentistry pages. When you’re ready for personal guidance, Request a Video Consult and we’ll talk through your options in a calm, low-pressure way.